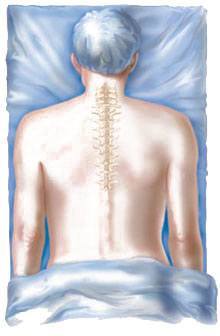
 Cervical foraminotomy is a surgical procedure done to relieve the symptoms of a pinched nerve by enlarging the neural foramen, and it can be performed in a minimally invasive way.
Cervical foraminotomy is a surgical procedure done to relieve the symptoms of a pinched nerve by enlarging the neural foramen, and it can be performed in a minimally invasive way.
The neural foramen is the opening by means of which a nerve root exits the spine to travel to skin, muscle and other tissues which it supplies. Herniated discs, bone spurs and thickened ligaments or joints can all cause narrowing of the neural foramen and cause painful symptoms.
Such symptoms may include neck pain, stiffness, and pain radiating into the shoulder, arm, and hand, as well as numbness, tingling and/or weakness in the arm and hand.
Patients who do not improve with conservative treatment may be candidates for surgery. Cervical foraminotomy is one of the surgical procedures that may be done to enlarge that passageway.
Dr. Rosenberg will always explain your non-surgical option (if there is one) as well as the surgical option along with its success rate, failure rate and risks. Except when cancer or dangerous spinal instability is present, it is always Dr. Rosenberg’s advice that if you are then not sure about having surgery, you should choose not to have surgery for the moment. Stop, think, and let some time pass, and the correct way for you to manage your condition will become clear.
How is it done?
The operation is performed with the patient on his or her stomach.
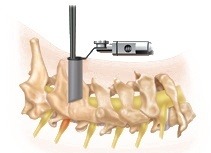
A small incision is made on the symptomatic side of the neck. Next, the muscles are gradually dilated and a tubular retractor is placed to give the surgeon access to the spine.
Bone or disc material and/or thickened ligaments are then removed to decompress and relieve pressure on the spinal cord and/or nerves.
The tubular retractor is removed, allowing the dilated muscles to come back together.
The incision is closed, and in most instances results in only a small scar.
Are There Any Potential Risks Or Complications?
Any surgery and anaesthesia can result in injury or even, rarely, death. One only has to read the newspaper to confirm that fact. Complications such as infection, nerve damage, blood clots, blood loss and bowel and bladder problems, along with complications associated with anaesthesia, are some of the potential risks of spinal surgery. A potential risk inherent to spinal fusion is failure of the vertebral bone and graft to properly fuse, a condition that may require additional surgery.
Dr. Rosenberg will tell you the types and magnitudes of risks for you undergoing a given procedure.
The sorts of complications which can occur with surgery to the back of the cervical spine include the following:
- Implant failure
- Infections
- Neck and/or arm pain
- Nerve or spinal cord injury, possibly causing impairment or paralysis
- Development or progression of disease at other cervical levels
- Bleeding or collection of clotted blood (hematoma)
- Reactions to anaesthesia
After Surgery
This minimally invasive procedure typically allows many patients to be discharged the same day of surgery; however, some patients will require a longer hospital stay. Most patients will notice immediate improvement of some or all of their symptoms; however, other symptoms may improve more gradually.
A positive attitude, reasonable expectations and compliance with your doctor’s post-surgery instructions all may contribute to a satisfactory outcome. Many patients are able to return to their regular activities within several weeks.
It is important that you discuss the potential risks, complications, and benefits of spinal surgery with your doctor prior to receiving treatment, and that you rely on your physician’s judgment. Only your doctor can determine whether you are a suitable candidate for this treatment.
