Cervical artificial disc replacement surgery is a joint replacement procedure that involves inserting an artificial disc between the vertebrae to replace a natural spinal disc after it has been removed.
A cervical artificial disc is a prosthetic device designed to maintain motion in the treated vertebral segment. A cervical artificial disc essentially functions like a joint, allowing for flexion, extension, side bending and rotation. Some newer discs are compressible, and actually function like shock-absorbers, as do natural discs.
One problem about artificial discs of all types, however, is that we can only guess at how they will behave in the spine afters years of use. We try to make an educated guess from millions of cycles of bench-testing in the laboratory, but the only real proof will emerge over the next 20 years or so.
Why Might I Need This Procedure?
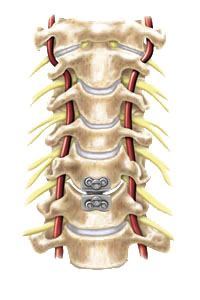
The intervertebral discs of the cervical spine are very important for the normal mobility and function of your neck. When healthy, they act as “cushions” for the individual bones of the spine, or vertebrae. Each disc is made up of two parts
- The nucleus pulposus – the soft, gel-like center of the disc
- The annulus fibrosis – strong, fibrous outer ring that surrounds and supports the nucleus pulposus
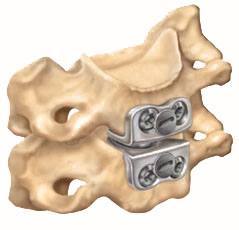
Over time, discs can become dried out, deflated or otherwise damaged, due to age, genetics and everyday wear-and-tear. When this happens, the nucleus pulposus may push through the annulus fibrosis. Disc degeneration also may result in boney spurs, also called osteophytes. If disc or bone material pushes into or impinges on a nearby nerve root and/or the spinal cord, it may result in pain, numbness, weakness, muscle spasms or loss of coordination, both at the site of the damage and elsewhere in the body, since most the nerves to the rest of the body (e.g., arms, chest, abdomen and legs) pass from the brain through the neck. Similar symptoms, however, may occur suddenly if the disc nucleus dislodges acutely and causes nerve root compression, a condition referred to as a herniated disc.
When non-surgical therapies fail to provide relief from your symptoms, Dr. Rosenberg may recommend spine surgery. The goal of cervical artificial disc surgery is to remove all or part of a damaged cervical disc (discectomy), relieve pressure on the nerves and/or spinal cord (decompression) and to preserve spinal alignment, whilst restoring mobility.
Not everyone with symptoms of disc degeneration in the neck is suitable for implantation of an artificial disc. In fact, more people need an anterior interbody fusion than are suitable for an artificial disc.
Dr. Rosenberg will advise which treatment is right for you, if sooner or later you are forced to resort to surgery.
Cervical artificial disc replacement surgery may be an appropriate treatment option for you if:
- You have been diagnosed with cervical radiculopathy, myelopathy or both with the presence of disc herniation and/or bone spurs
- Your disc has not deflated to such an extent that it has lost more than 50% of its original height
- The facets joints at the back of the spine at that level do not show degenerative changes (wear and tear)
- Your symptoms did not improve after conservative treatment measures, which usually include: abandoning harmful neck exercises and manipulations, walking for exercise, avoidance of soft chairs and watching TV lying down, and strict attendance to erect sitting
- You require treatment at only one cervical level
- You are at least 18 years of age with skeletal maturity
- You are not pregnant
Dr. Rosenberg will always explain your non-surgical option (if there is one) as well as the surgical option along with its success rate, failure rate and risks. Except when cancer or dangerous spinal instability is present, it is always Dr. Rosenberg’s advice that if you are then not sure about having surgery, you should choose not to have surgery for the moment. Stop, think, and let some time pass, and the correct way for you to manage your condition will become clear.
How Is Cervical Artificial Disc Replacement Surgery Performed?
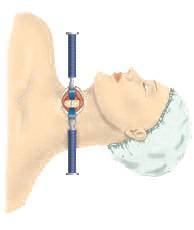
Through a small incision made near the front of your neck (a surgical approach called the anterior approach) your surgeon will:
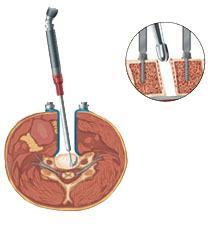
- Gently pull aside the soft tissues – skin, fat and muscle – as well as the trachea (windpipe) and oesophagus (the tube down which you swallow) to access the cervical spine
- Remove the disc and bone material from around the neural structures to relieve the pressure on them
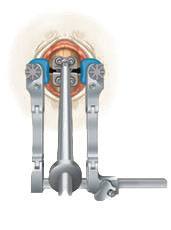
- Insert and secure the artificial disc into the intervertebral space, using specialized instruments
- Ease the soft tissues of the neck and other structures back into place and
- Close the incision
 |
 |
 |
How Long Will It Take Me To Recover?
Dr. Rosenberg will advise you in detail on the post-operative recovery/exercise plan to help you return to your normal activity level as soon as possible. The amount of time that you have to stay in the hospital will depend on this treatment plan. You typically will be up and walking in the hospital by the end of the first or second day after the surgery. You may return to work in 3-6 weeks, depending on how well your body is healing and the type of work/activity level you plan to return to.
Every patient is different, however, and Dr. Rosenberg will determine the appropriate recovery protocol for you. Please note that much of this advice is for your safety, and thus it is important that you follow it to the letter.
Are There Any Potential Risks Or Complications?
Any surgery and anaesthesia can result in injury or even, rarely, death. One only has to read the newspaper to confirm that fact. Complications such as infection, nerve damage, blood clots, blood loss and bowel and bladder problems, along with complications associated with anaesthesia, are some of the potential risks of spinal surgery. A potential risk inherent to spinal fusion is failure of the vertebral bone and graft to properly fuse, a condition that may require additional surgery.
Dr. Rosenberg will tell you the types and magnitudes of risks for you undergoing a given procedure.
The sorts of complications which can occur with surgery to cervical spine include the following:
- Implant failure
- Infections
- Neck and/or arm pain
- Difficulty swallowing
- Voice Hoarseness
- Nerve or spinal cord injury, possibly causing impairment or paralysis
- Development or progression of disease at other cervical levels
- Bleeding or collection of clotted blood (hematoma)
- Reactions to from anaesthesia
